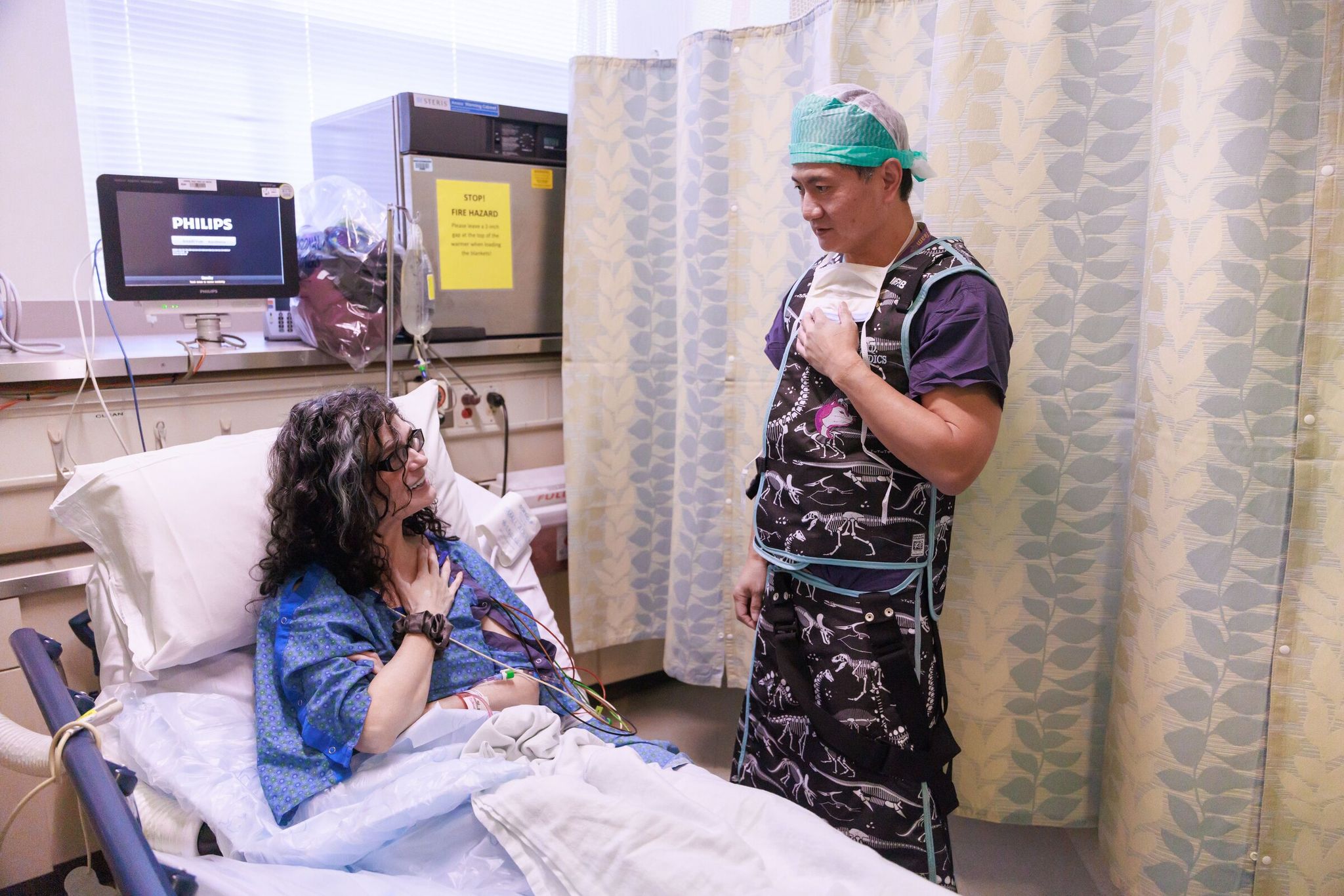
After a decade of fighting debilitating pain, Seattle resident Erika Clancy became one of the first patients in the region to receive a revolutionary thumb joint replacement. The procedure, the first in the U.S. Pacific Northwest, was successfully performed by a surgical team from UW Medicine — the University of Washington’s academic medical system and one of the region’s leading medical centers. Innovative procedures like this are often done here because the system combines a medical school, research institutes and clinical practice, with access to advanced technologies and research funding.
Erika, a 51-year-old former teacher, suffered from arthritis at the base of the thumb, known as carpometacarpal (CMC) arthritis. This degenerative condition wears away cartilage, affects up to a third of postmenopausal women, and makes the simplest actions — from shaking hands to washing dishes — agonizing.
Over the past decade Clancy underwent six hand surgeries, wore splints and regularly received cortisone injections, but traditional surgical approaches in the U.S. often meant long recoveries without a guarantee of full strength or motion return.
Hope arrived three years ago when her doctor mentioned a new method popular in Europe — implantation of a metal-polyethylene joint prosthesis. In summer 2023 the U.S. Food and Drug Administration (FDA) approved the procedure for use in the country.
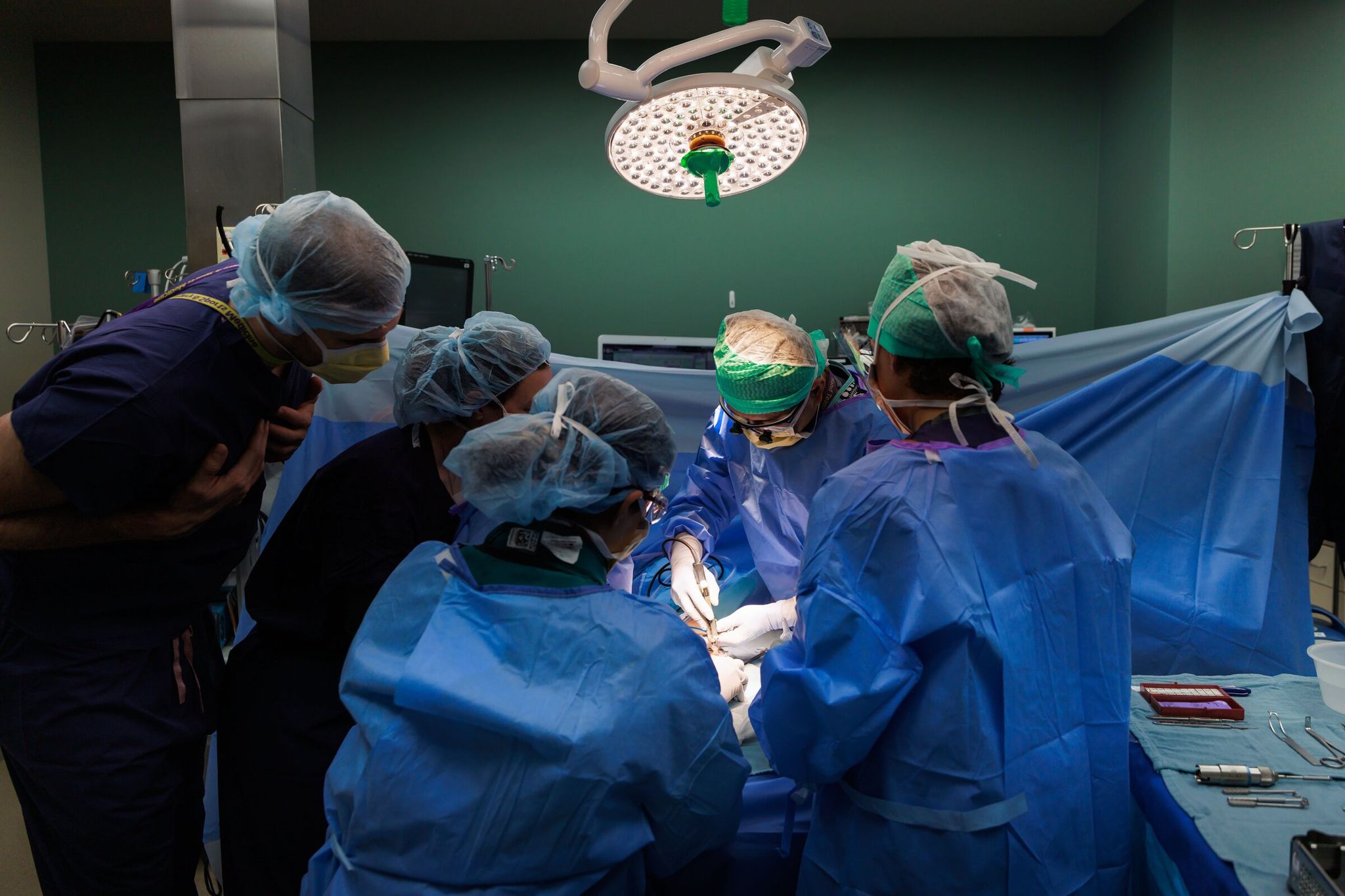
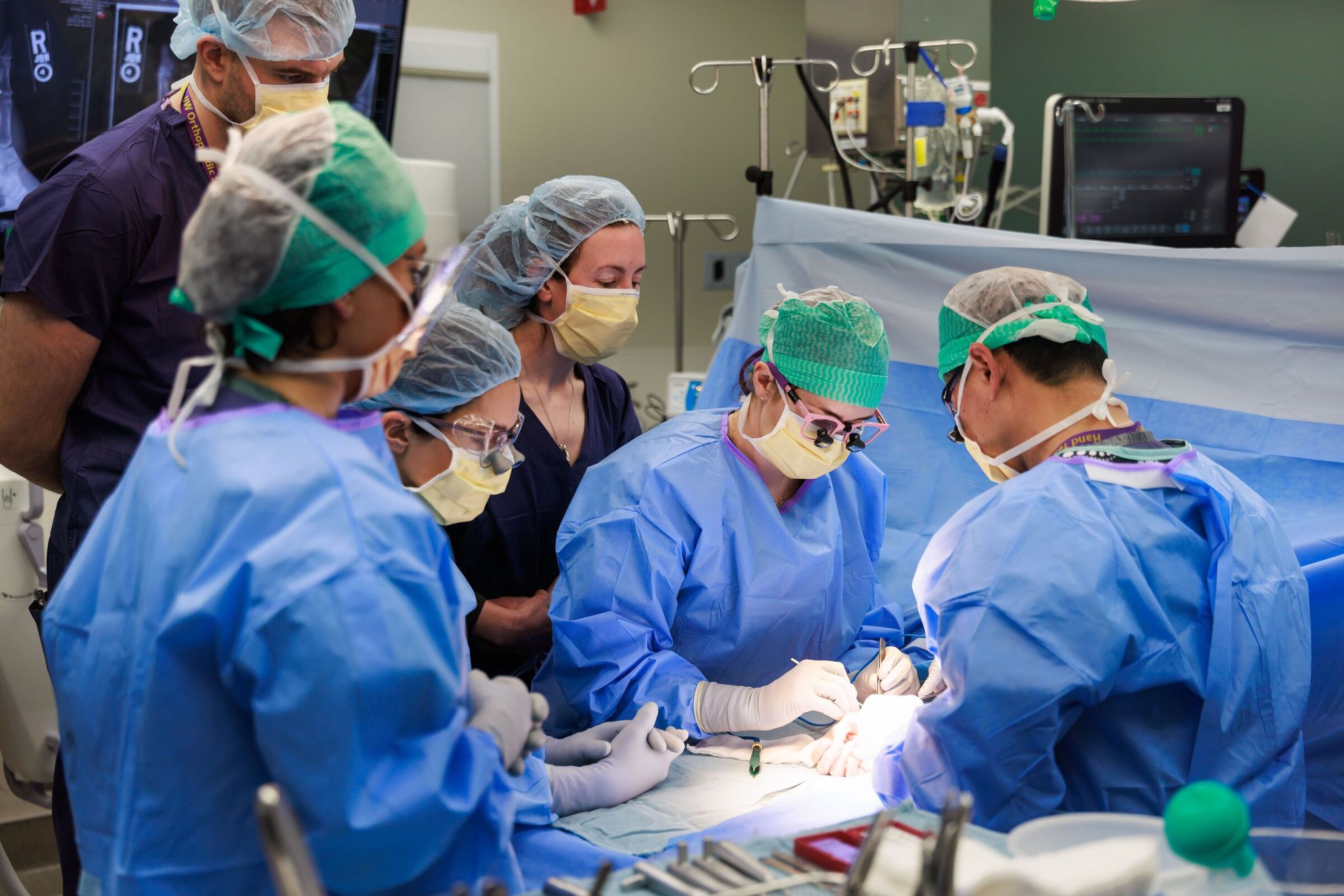
The operation was led by Dr. Jerry Huang, an associate professor of surgery at the University of Washington who specializes in minimally invasive procedures. He was one of roughly 45 U.S. surgeons invited by the Swiss manufacturer KeriMedical to train in Europe before the technology launched in the United States. His selection for training likely related to his specialty and experience, as well as UW Medicine’s practice of sending leading clinicians to learn new techniques at world centers of excellence. The procedure is already considered the gold standard of care in Europe.
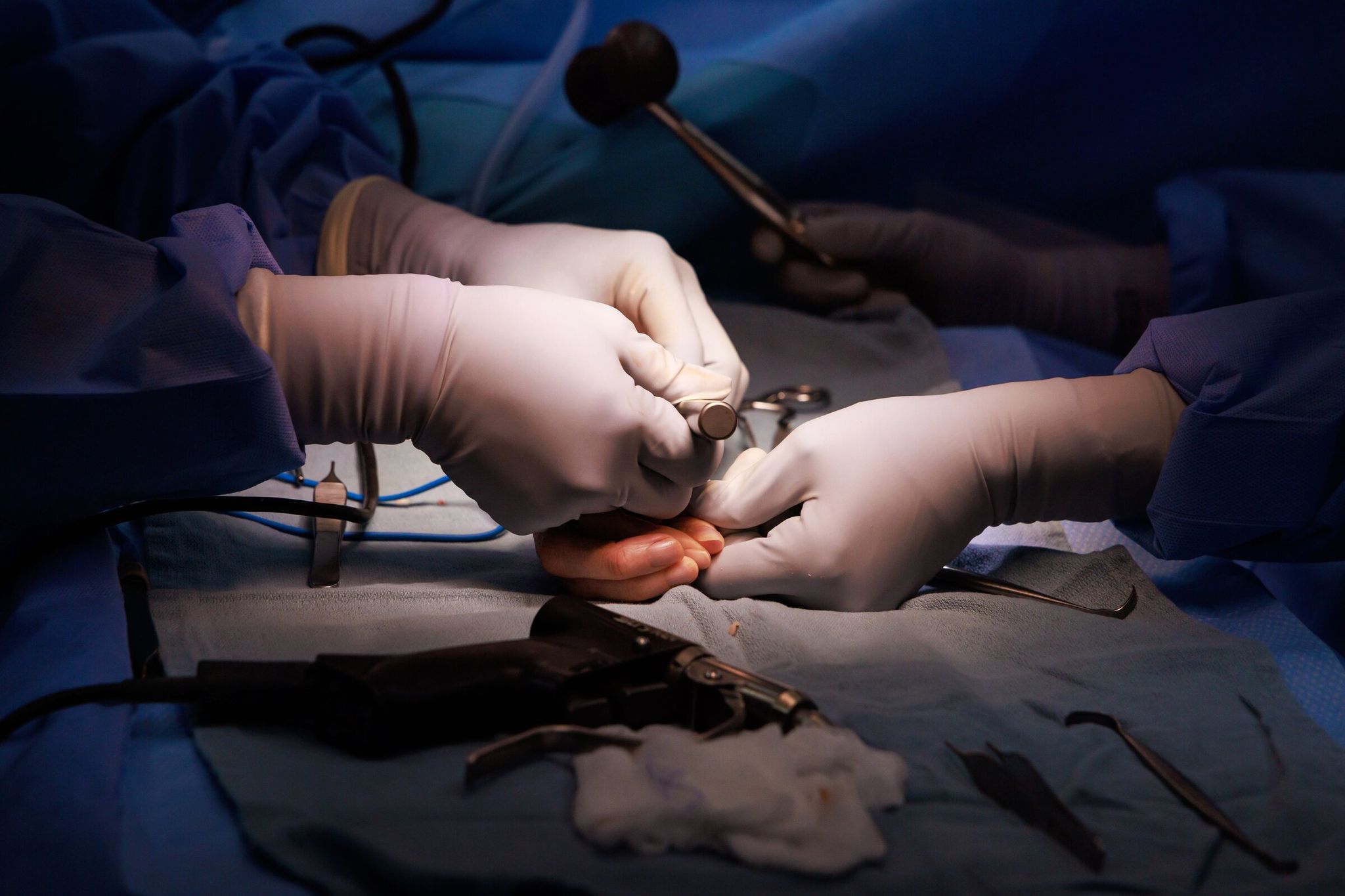
The procedure itself, which Dr. Huang compares to a “mini hip replacement,” involves removing the arthritis-damaged joint and implanting a prosthesis that connects the two main bones of the thumb — the metacarpal and the trapezium. This is intended to provide stability and a wide range of motion.
The thumb’s anatomy is incredibly complex — it must move in multiple planes to provide gripping and pinching motion. That’s why its arthritis so severely limits patients and why joint replacement is a technically demanding task for surgeons.
Clancy’s surgery was performed at the UW medical center, part of a large academic hospital complex that includes several hospitals and combines care, teaching and research. The procedure took about 45 minutes and, according to Dr. Huang, went “very smoothly.” After the implant was placed and a dressing applied, the patient went home to recover in Bellevue — a separate city east of Seattle but part of the same metropolitan area — just an hour after surgery. Patients often choose to recover in Bellevue because of rehabilitation centers and a calmer atmosphere, while remaining within the same UW Medicine network that serves the region.
According to Medartis, which now owns the technology, about 300 such implants have been placed in the U.S. since September. The goal is to train more surgeons over the coming years and make the operation the new standard of care for CMC arthritis in the country.
Being “first in the region” for medical procedures is relatively common in Seattle thanks to the concentration of research institutes, biotech companies and proximity to tech giants that invest in medical innovation.
Clancy is now recovering at home. She will wear a plaster splint for the first two weeks, then begin physical therapy. In three months, Dr. Huang promised, she should have no activity restrictions. Asked about her expectations, Erika smiled and gave a thumbs-up — now, pain-free.
Based on: Seattle doctor becomes first in PNW to perform new thumb surgery